In recent years there has been renewed interest in immunotherapies to treat of metastatic renal cell carcinoma (mRCC). Immunotherapies increase the body’s natural finely regulated multiple-step anti-tumour immune response (Figure 1). The balance of stimulatory and inhibitory signals (reviewed in Chen & Mellman, 2013) are important in maintaining self-tolerance and modulating normal immune responses to minimising health tissue damage. However, tumours can develop mechanisms to evade this immune response.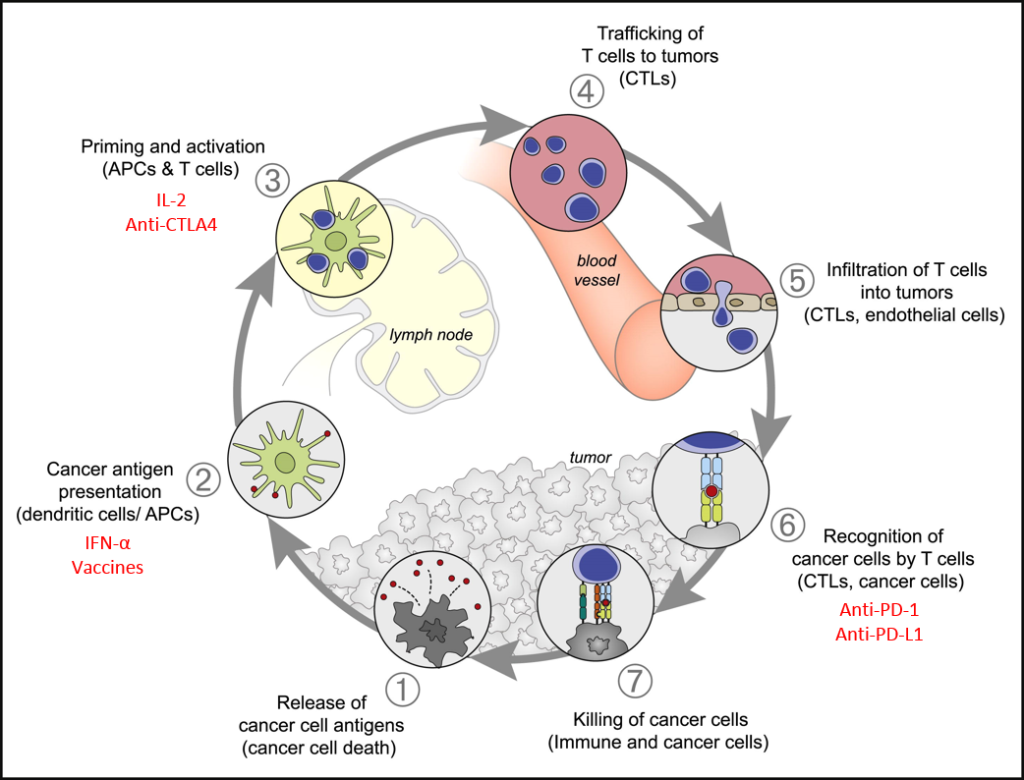
Figure 1: Immune Response Cycle. The major steps in the immune response cycle to cancer cells. Immunotherapies target a number of different steps (red). Modified from Chen & Mellman (2013) Immunity 39, 1-10.
The approved immunotherapies for RCC are the cytokines Interferon-alpha (IFN-α) and Interleukin-2 (IL-2) to stimulate T-cell activity. Unfortunately this can result in a variety of treatment related toxicities. The response rate to these drugs is relatively low but the responses are more likely to be durable. An alternative strategy is to inhibit specific immune checkpoints that normally act to limit excessive immune activity. The numerous stimulatory and inhibitory checkpoints in the immune system minimise the death of healthy, “self” cells in an immune response. The presence of inhibitory signals on tumour cells can therefore stop an immune response but the blockade of these inhibitory signals can increase the immune response and tumour cell death. A list of ongoing trials is available here.
One such inhibitor is Cytotoxic T-Lymphocyte Antigen 4 (CTLA-4) which when bound to B7-1 or B7-2 disrupts early T-cell activation and blocks cytokine production. Ipilumumab binds to CTLA-4 and blocks this inhibition resulting in increased production of auto-reactive T-cells and cytokines. While some patients have responded well to ipilumumab there are some severe adverse events (AE) associated with off-target effects of this drug (Yang et al., 2007).
A different checkpoint target is the Programmed cell Death-1 (PD-1)/PD-L1 inhibitory signalling pathway which reduces T-cell signalling and activation helping to maintain peripheral tolerance. Anti-PD-1 antibodies – nivolumab, pembrolizumab and pidilizumab – and the anti-PD-L1 antibody MPDL3280A are effective at blocking this signalling. PD-1 is expressed on a range of immune cells and PD-L1 can be expressed by tumour cells minimising the immune response. Nivolumab is the most frequently used anti-PD-1 in RCC and early phase trials have shown enhanced long-term survival (Lipson et al., 2013), with varied doses of nivolumab inducing comparable response rates with manageable toxicity profiles (Motzer et al., 2015). There are also numerous ongoing trials investigating pembrolizumab which showed some response in melanoma patients but can have severe AE (Martin-Liberal et al., 2015).
An alternative, and potentially complimentary, approach would be the use of cancer vaccines to prime the immune system for response to cancer cells. The introduction of antigen presenting cells (APCs) loaded with tumour-derived RNA, such as AGS-003, induces a tumour-specific immune response (Amin et al., 2015). A synthetic vaccine, IMA901, consists of 10 Tumour Associated Peptides (TUMAPs) bound to HLA ligands for presentation to the immune system and as in early trials (Bedke & Stenzl, 2013).
The immune related AEs (irAE) seen in immunotherapy drug trials can differ from AE from other drug types and can be severe (Weber et al., 2012). Early diagnosis and effective toxicity management is required to ensure ongoing treatment is tolerable. Early trials suggest a correlation between response rate and frequency of irAEs and perhaps such irAEs could be worth enhanced survival. Further trials will also determine any risk of sequential toxicities that could impact on treatment regimens.
In addition to the development of therapies there is also a great need for research into relevant biomarkers; currently there are only indicative and not predictive biomarkers to determine which patients are most likely to response. Patient selection could also reduce the use of ineffective treatments which have a high irAE risk but no or minimal health benefit. Patient fitness and toxic burden also needs to be considered as frailer patients may not be able to tolerate AEs or to survive an initial decline before response begins.
As immunotherapies develop they may also be beneficial as adjuvant treatments following surgical resection. The responses to immunotherapies can be durable, continuing long after treatment has completed indicating the formation of tumour specific immune memory; they could therefore also be useful in reducing recurrence risk in high risk patients such as those with hereditary forms of RCC.
- Amin A, Dudek AZ, Logan TF, Lance RS, Holzbeierlein JM, Knox JJ, Master VA, Pal SK, Miller WH Jr, Karsh LI, Tcherepanova IY, DeBenedette MA, Williams WL, Plessinger DC, Nicolette CA, Figlin RA (2015). Survival with AGS-003, an autologous dendritic cell-based immunotherapy, in combination with sunitinib in unfavorable risk patients with advanced renal cell carcinoma (RCC): Phase 2 study results. J Immunother Cancer Apr 21;3:14. PMID: 25901286.
- Bedke J, Stenzl A (2013) IMA901: a peptide vaccine in renal cell carcinoma. Expert Opin Investig Drugs Oct;22(10):1329-36. Review. PMID: 23899354.
- Chen DS, & Mellman I (2013). Oncology meets immunology: the cancer-immunity cycle. Immunity, 39 (1), 1-10 PMID: 23890059.
- Lipson EJ, Sharfman WH, Drake CG, Wollner I, Taube JM, Anders RA, Xu H, Yao S, Pons A, Chen L, Pardoll DM, Brahmer JR, Topalian SL (2013). Durable cancer regression off-treatment and effective reinduction therapy with an anti-PD-1 antibody. Clin Cancer Res Jan 15;19(2):462-8. PMID: 23169436.
- Martin-Liberal J, Kordbacheh T, Larkin J (2015). Safety of pembrolizumab for the treatment of melanoma. Expert Opin Drug Saf Apr 30:1-8. [Epub ahead of print] PMID: 25927979.
- Motzer RJ, Rini BI, McDermott DF, Redman BG, Kuzel TM, Harrison MR, Vaishampayan UN, Drabkin HA, George S, Logan TF, Margolin KA, Plimack ER, Lambert AM, Waxman IM, Hammers HJ (2015). Nivolumab for Metastatic Renal Cell Carcinoma: Results of a Randomized Phase II Trial. J Clin Oncol May 1;33(13):1430-7. PMID: 25452452.
- Weber JS, Kähler KC, Hauschild A (2012). Management of immune-related adverse events and kinetics of response with ipilimumab. J Clin Oncol Jul 20;30(21):2691-7. PMID: 22614989
- Yang JC, Hughes M, Kammula U, Royal R, Sherry RM, Topalian SL, Suri KB, Levy C, Allen T, Mavroukakis S, Lowy I, White DE, Rosenberg SA (2007). Ipilimumab (anti-CTLA4 antibody) causes regression of metastatic renal cell cancer associated with enteritis and hypophysitis. J Immunother Nov-Dec;30(8):825-30. PMID: 18049334.
In RCC, a lot of focus currently is on the nivolumab, MPDL3280A and Ipilumumab…
However in Sweden there is a biotech company called Immunicum that has an allogenic cancer vaccine (INTUVAX) that in combination with sunitinib most likely will result in better survival data than the combination of immune checkpoint inhibitors.
The Phase I/II study in kidney cancer (mRCC), combines INTUVAX with Sunitinib. The study has showed amazing survival in a small amount of patients. A total of 11 patients were recruited to the study, five patients with intermediate prognosis and six patients with poor prognosis, subgrouping according to so-called MSKCC criteria. The median overall survival after vaccination for the subgroup with poor prognosis is currently at 22 months and has thus already exceeded the expected median overall survival of 5 months with interferon treatment and 9 months with only Sunitinib treatment. The median overall survival for the intermediate patients is too early to comment on even if the patients already have lived surpassed expected survival.
I have a Non Confidential Slide deck if you want to have a look at the company. In case you want it please send me an email and I will try to send it to you a.s.a.p.
Did you know about this drug before this email?
Best Regards,
Kenneth Nord
It’s hard to find educated people on this subject, but you sound like you know what you’re talking
about! Thanks